Abstract
Objective
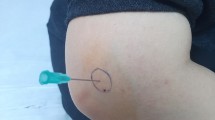
To evaluate whether autologous conditioned plasma offers any therapeutic advantage over ultrasound-guided dry needling as a stand-alone procedure in the treatment of refractory lateral epicondylitis.
Materials and methods
Prospective, randomized pilot study of 28 patients (11 men, 17 women, mean age, 49.1 years) with refractory lateral epicondylitis (mean symptom duration, 19.1 months) who underwent either dry needling (n = 13) or dry needling combined with autologous conditioned plasma (ACP) injection (n = 15). Each patient received two separate injections (0 weeks and 1 month) and analysis of visual analogue pain scores (VAS) and Nirschl scores were performed pre-procedure, at 2 months and final evaluation at 6 months. Successful treatment was defined as more than a 25 % reduction in pain scores without re-intervention. Data was analyzed using the Mann–Whitney test and local research ethics committee approval was obtained.
Results
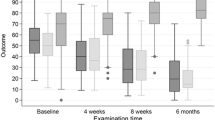
At 2 months, the mean VAS improvement was 0.85 (12.3 %) in the dry needling group compared to 2.19 (27.1 %) in the ACP group (p = 0.76) and there was a 5.83-point and 20.3-point Nirschl score improvement respectively (p = 0.72). At the final follow-up of 6 months, the mean VAS improvement was 2.37 (34 %) in the dry needling group compared to 3.92 (48.5 %) in the ACP group (p = 0.74) and there was a 22.5-point and 40-point Nirschl score improvement, respectively (p = 0.82).
Conclusions
There is a trend to greater clinical improvement in the short term for patients treated with additional ACP, however no significant difference between the two treatment groups was demonstrated at each follow-up interval. A larger, multicenter, randomized controlled trial is required to corroborate the results of this pilot study.





Similar content being viewed by others
References
Allander E. Prevalence, incidence and remission rates of some common rheumatic diseases and syndromes. Scand J Rheumatol. 1974;3:145–53.
Hudak P, Cole D, Haines T. Understanding prognosis to improve rehabilitation: the example of lateral elbow pain. Arch Phys Rehabil. 1996;77:568–93.
Creaney L, Wallace A, Curtis M, Connell D. Growth factor-based therapies provide additional benefit beyond physical therapy in resistant elbow tendinopathy: a prospective, double-blind, randomised trial of autologous blood injections versus platelet-rich plasma injections. Br J Sports Med. 2011;45:966–71.
Peerbooms JC, Sluimer J, Bruijn DJ, Gosens T. Positive effect of an autologous platelet concentrate in lateral epicondylitis in a double-blind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med. 2010;38:255–62.
Gosens T, Peerbooms JC, van Laar W, den Oudsten BL. Ongoing positive effect of platelet-rich plasma versus corticosteroid injection in lateral epicondylitis: a double-blind randomized controlled trial with 2-year follow-up. Am J Sports Med. 2011;39:1200–8.
Bisset L, Coombes B, Vicenzino B. Tennis elbow. Clinical Evidence BMJ Publishing Group Ltd 2011.
Radwan YA, ElSobhi G, Badawy WS, Reda A, Khalid S. Resistant tennis elbow: shock-wave therapy versus percutaneous tenotomy. Int Orthop. 2008;32:671–7.
Dingemanse R, Randsdorp M, Koes BW, Huisstede BM. Evidence for the effectiveness of electrophysical modalities for treatment of medial and lateral epicondylitis: a systematic review. Br J Sports Med 2013 Jan 18. [Epub ahead of print]
Lewis M, Hay EM, Paterson SM, Croft P. Local steroid injections for tennis elbow: does the pain get worse before it gets better? Results from a randomized controlled trial. Clin J Pain. 2005;21(4):330–4.
Assendelft WJ, Hay EM, Adshead R, Bouter LM. Corticosteroid injections for lateral epicondylitis: a systematic overview. Br J Gen Pract. 1996;46(405):209–16.
Smidt N, van der Windt DA, Assendelft WJ, Deville WL, et al. Corticosteroid injections, physiotherapy, or a wait-and-see policy for lateral epicondylitis: a randomised controlled trial. Lancet. 2002;359:657–62.
Bisset L, Beller E, Jull G, Brooks P, Darnell R, et al. Mobilisation with movement and exercise, corticosteroid injection, or wait and see for tennis elbow: randomised trial. BMJ. 2006;333(7575):939.
Buchbinder R, Johnston RV, Barnsley L, Assendelft WJJ, Bell SN, Smidt N. Surgery for lateral elbow pain. Cochrane Database Syst Rev. 2011;(3)CD003525. doi:10.1002/14651858.CD003525.pub2.
McShane JM, Shah VN, Nazarian LN. Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow: is a corticosteroid necessary? J Ultrasound Med. 2008;27:1137–44.
James SL, Ali K, Pocock C, Robertson C, Walter J, et al. Ultrasound guided dry needling and autologous blood injection for patellar tendinosis. Br J Sports Med. 2007;41:518–22.
Alsousou J, Thompson M, Hulley P, Noble A, et al. The biology of platelet-rich plasma and its application in trauma and orthopaedic surgery. J Bone Joint Surg. 2009;91(8):987–96.
Connell D, Ali K, Ahmad M, Lambert S, Corbett S, Curtis M. Ultrasound-guided autologous blood injection for tennis elbow. Skeletal Radiol. 2006;35:371–7.
Chaudhury S, de La Lama M, Adler RS, Gulotta LV, Skonieczki B, Chang A, et al. Platelet-rich plasma for the treatment of lateral epicondylitis: sonographic assessment of tendon morphology and vascularity (pilot study). Skeletal Radiol. 2013;42:91–7.
Thanasas C, Papadimitriou G, Charalambidis C, Paraskevopoulous I, Papanikolaou A. Platelet-rich plasma versus autologous whole blood for the treatment of chronic lateral elbow epicondylitis: a randomized controlled clinical trial. Am J Sports Med. 2011;39:2130–4.
Urbaniak GC, Plouse S. Research Randomizer (Version 4.0) [Computer software]. Retrieved on June 22, 2013, from http://www.randomizer.org.
Nirschl RP. Elbow tendinosis/tennis elbow. Clin Sports Med. 1992;11(4):851–70.
Kraushaar BS, Nirschl RP. Tendinosis of the elbow. Clinical features and findings of histological, immunohistochemical and electron microscopy studies. J Bone Joint Surg Am. 1999;81:259–78.
Krogh TP, Fredberg U, Stengaard-Pedersen K, Christensen R, Jensen P, Ellingsen T. Treatment of lateral epicondylitis with platelet-rich plasma, glucocorticoid, or saline: a randomized, double-blind, placebo-controlled trial. Am J Sports Med. 2013;41:625–35.
Weibrich G, Kleis WKG, Hafner G, Hitzler W. Growth factor levels in platelet-rich plasma and correlations with donor age, sex and platelet count. J Cran- Max Surg. 2002;30:97–102.
Arthrex ACP Double Syringe System Autologous Conditioned Plasma [homepage on the internet]. Available from: http://www.deviceinnovation.com/images/sub_1332905727/Arthrex-ACP-Double-Syringe-System.pdf.
Marx RE. Platelet-rich plasma: evidence to support its use. J Oral Maxillofac Surg. 2004;62:489–96.
Foster TE, Puskas BL, Mandelbaum BR, Gerhardt MB, Rodeo SA. Platelet-rich plasma: from basic science to clinical applications. Am J Sports Med. 2009;37:2259–72.
Nirschl RP, Pettrone FA. Tennis elbow: the surgical treatment of lateral epicondylitis. J Bone Joint Surgery Am. 1979;61:832–9.
Boyd HB, McLeod Jr AC. Tennis elbow. J Bone Joint Surg Am. 1973;55:1183–7.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stenhouse, G., Sookur, P. & Watson, M. Do blood growth factors offer additional benefit in refractory lateral epicondylitis? A prospective, randomized pilot trial of dry needling as a stand-alone procedure versus dry needling and autologous conditioned plasma. Skeletal Radiol 42, 1515–1520 (2013). https://doi.org/10.1007/s00256-013-1691-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-013-1691-7